Why
sperm health
matters.
3 reasons sperm quality is now in the spotlight.
1
About 40% of the time, a couple’s infertility issue is caused by the male, and that percentage is on the rise.
2
Sperm counts have plummeted more than 50% over the last four decades, according to the most comprehensive analysis of over 7,000 studies of Western male patients.
3
Couples are delaying having children, and once past the age of 35 or 40, a male’s sperm quality may be naturally on the decline, which accelerates the importance to adopt habits and solutions that do not decrease the quality of his sperm any further.

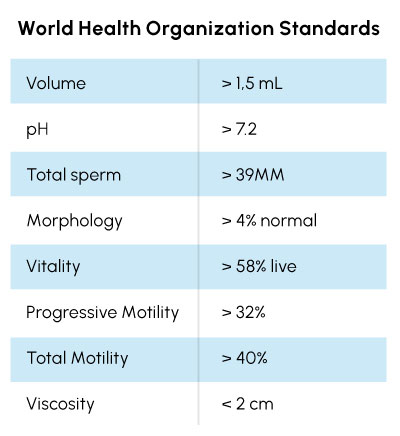
How sperm health is measured.
If you have been trying to conceive naturally for 12 months or longer without success. it’s important you ask your doctor for a semen analysis as early in the process as possible. Analysis requires the male partner to provide a semen sample, and he may be required to do more than one sampling to confirm initial results.
Standard parameters measured for analysis include volume, pH, count, motility (ability to swim), morphology (shape), and more. Some of these results are affected by his genetics, diet, lifestyle, habits, and even his environment. Ask your doctor what you can do to improve your sperm quality.
The importance of the acrosome.
Standard semen parameters like motility and forward progression are excellent visible indicators for sperm health. However, acrosome membrane data is crucial for a final assessment. Sperm have a helmet-like covering called the acrosome, which contains enzymes that break down the protective coating of a female’s egg. The acrosome allows the sperm to eventually penetrate and fertilize the egg.
When it comes to assisted reproductive technologies, we are learning just how crucial intact acrosomes are. If the sample sperm are highly motile yet have a low percentage of intact acrosome membranes, their likelihood to penetrate through the egg’s protective coating to fertilize the egg decreases significantly.

Intact Acrosome
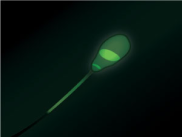
Broken Acrosome
What causes sperm damage during collection and how to prevent it.
After analysis, semen sample collection is the initial step in an assisted fertility procedure (IUI, IVF, ICSI). Typically, the male partner collects in a generic specimen cup, which leaves his sperm susceptible to damage right away. Its thin walls, cheap plastic material, and large flat bottom leave sperm completely unprotected within a dry container.
The type of damage that can occur during collection.
Thermal Shock
Severe temperature fluctuations damage critical sperm membranes and activate the sperm to use all its energy before it’s actually ready for the assisted fertility procedure.
pH Imbalance
When a semen sample remains in a dry container, cellular waste creates an environment that is too acidic (pH 6.2 and lower), which interferes with motility and decreases the percentage of total motile sperm.
Pressure Imbalance
This manifests itself as visible swelling or dehydration of the sperm, which may affect critical membrane integrity, and occurs when not enough or too much fluid accompanies the sample.